Postpartum Recovery: Physical Therapy for Pelvic Health After Birth
The postpartum period marks a time of significant physiological adjustment for individuals following childbirth. Pregnancy and delivery, whether vaginal or via Caesarean section, place considerable demands on the body, leading to numerous physical changes that require time and attention for optimal recovery. Addressing these changes effectively supports long-term health and well-being.
Pelvic health is a crucial, yet frequently underemphasized, component of postpartum recovery. The structures within the pelvis, including muscles, ligaments, and connective tissues, undergo substantial stress during pregnancy and birth. Physical therapy focused on pelvic health offers targeted strategies to manage and rehabilitate these structures, addressing common postpartum concerns and promoting a return to comfortable function. Seeking guidance from a pelvic floor physical therapist can facilitate a smoother, more informed recovery journey.
Common Postpartum Physical Changes
The body undergoes a complex recovery process after childbirth. Several common physical changes occur, particularly affecting the pelvic region and core musculature. Understanding these changes is the first step towards addressing them appropriately.
-
- Urinary Incontinence: The involuntary leakage of urine affects a significant number of individuals after childbirth. This can range from occasional leakage during activities like coughing or sneezing (stress incontinence) to a sudden, strong urge to urinate (urge incontinence). Pregnancy and delivery can stretch and weaken pelvic floor muscles, affecting urethral support and closure mechanisms.
- Pelvic Organ Prolapse (POP): POP occurs when pelvic organs, such as the bladder, uterus, or rectum, descend from their normal position into the vaginal canal. This results from weakened pelvic floor muscles and connective tissues that normally support these organs. Symptoms can include a feeling of heaviness or bulging in the vagina, discomfort, or difficulty with urination or bowel movements.
-
- Diastasis Recti Abdominis (DRA): This condition involves the separation of the rectus abdominis muscles (the “six-pack” muscles) along the linea alba, the connective tissue running down the midline of the abdomen. It commonly occurs during pregnancy as the uterus expands. While some separation is normal, significant or persistent DRA can affect core stability, contribute to back pain, and alter abdominal appearance.
- Perineal Tearing and Scar Tissue: The perineum, the area between the vagina and anus, can tear naturally during vaginal delivery or may be surgically cut (episiotomy). Healing involves scar tissue formation, which can sometimes lead to pain, tightness, or discomfort, particularly during intercourse (dyspareunia) or with pressure. Proper management of scar tissue is important for restoring tissue mobility and reducing associated symptoms.
- Pelvic Girdle Pain (PGP): Pain experienced in the joints of the pelvis (sacroiliac joints at the back or the pubic symphysis at the front) is common during pregnancy and can persist postpartum. Hormonal changes affecting ligament laxity, altered biomechanics, and muscle imbalances contribute to PGP. This pain can interfere with walking, standing, and other daily activities.
The Role of Physical Therapy in Postpartum Pelvic Health
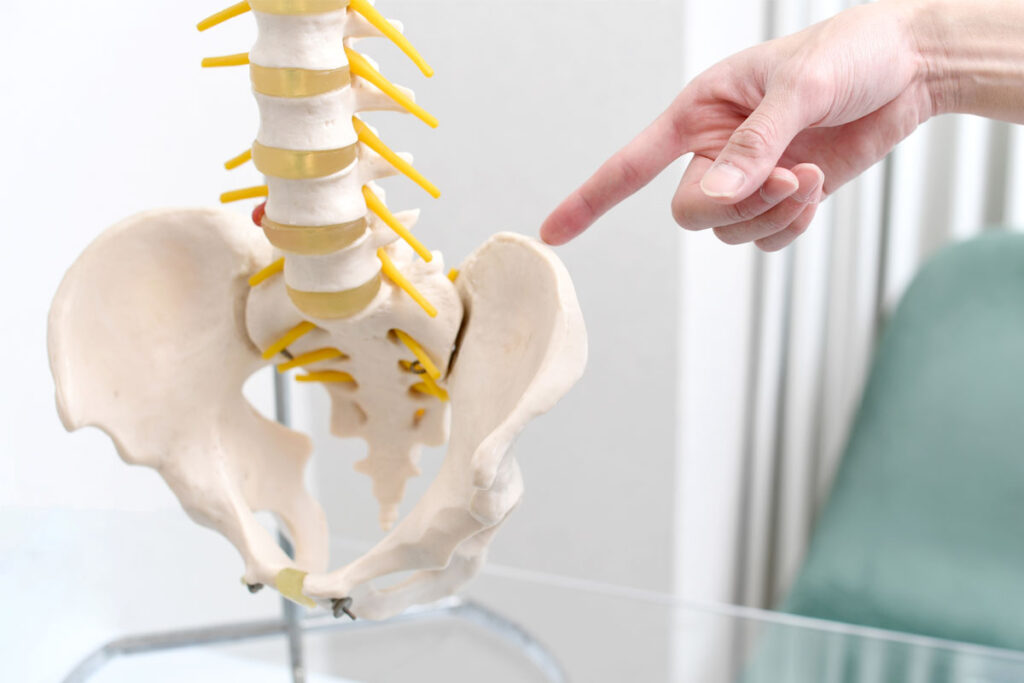
Physical therapy addresses postpartum musculoskeletal challenges, with pelvic health therapists assessing and treating conditions related to the pelvic floor and core, promoting recovery and preventing long-term complications.
- Comprehensive Assessment: Physical therapists conduct detailed evaluations, including health history, assessment of posture, core strength, breathing patterns, and pelvic floor function. This often involves both external and internal examinations (with consent) to accurately identify muscle strength, endurance, coordination, tissue condition, and any specific impairments contributing to symptoms.
- Pelvic Floor Muscle Training: Contrary to common belief, treatment involves more than just Kegel exercises. Therapists provide individualized instruction on correctly contracting, relaxing, and coordinating pelvic floor muscles. Training addresses strength, endurance, timing, and the ability to integrate pelvic floor activation with other core muscles and daily movements, tailored to specific conditions like incontinence or prolapse.
- Core Muscle Rehabilitation: Addressing issues like diastasis recti and general core weakness is fundamental. Physical therapists guide individuals through exercises designed to progressively strengthen deep abdominal muscles (like the transversus abdominis), back muscles, and the diaphragm, coordinating them with the pelvic floor for optimal stability and function.
- Manual Therapy Techniques: Hands-on techniques may be employed to address various issues. This can include soft tissue release for tight or painful muscles (pelvic floor, hips, abdomen), joint mobilization for pelvic girdle pain, and scar tissue massage (perineal or C-section scars) to improve tissue mobility and reduce pain or restriction.
- Education and Self-Management Strategies: A significant component involves educating individuals about their condition, proper body mechanics for activities like lifting and childcare, bladder and bowel health habits (including fluid/diet advice), pain management techniques, and strategies for a gradual return to exercise and desired activities, empowering them in their recovery.
- Management of Pelvic Pain: For conditions like dyspareunia (painful intercourse) or persistent pelvic pain, physical therapy offers strategies including manual therapy, specific exercises to relax or strengthen muscles, biofeedback, and pain neuroscience education to help manage and reduce pain sensitivity and improve function.
- Guidance on Return to Activity/Exercise: Physical therapists provide crucial guidance on safely resuming physical activities and exercise postpartum. They help individuals understand appropriate timelines, exercise modifications, and progressions based on their specific recovery status, minimizing the risk of injury or symptom exacerbation.
What to Expect During a Postpartum Pelvic Health Physical Therapy Session
Postpartum recovery pelvic health physical therapy sessions are tailored to each individual’s unique history, symptoms, and goals, ensuring a comprehensive and personalized approach.
- Detailed History Taking: The therapist will begin by discussing your pregnancy, labour, and delivery experience in detail. They will ask about your current symptoms (pain, incontinence, pressure), bladder and bowel function, sexual health concerns, activity levels, and overall recovery goals. This information provides crucial context.
- Postural and Movement Assessment: An evaluation of your posture, gait (walking pattern), and functional movements (like squatting, lifting, or bending) will be performed. The therapist observes how your body moves and identifies any compensatory patterns, muscle imbalances, or alignment issues contributing to your symptoms.
- External Musculoskeletal Examination: The therapist will assess the muscles and joints of your lower back, hips, and pelvis externally. This includes checking for tenderness, muscle tightness or weakness, joint mobility restrictions, and assessing the abdominal muscles for diastasis recti abdominis (DRA).
- Internal Pelvic Floor Muscle Assessment (Optional but Recommended): With your informed consent, the therapist may perform an internal vaginal and/or rectal examination. This allows for direct assessment of pelvic floor muscle strength, endurance, coordination, tone (resting tension), and the presence of trigger points or scar tissue restrictions. This provides invaluable information for targeted treatment.
- Explanation of Findings: Following the assessment, the therapist will clearly explain their findings in understandable terms. They will discuss how the assessment relates to your specific symptoms and outline the proposed treatment plan, ensuring you understand the rationale behind their recommendations.
- Personalized Treatment Plan Development: Based on the assessment findings and your goals, a tailored treatment plan will be created. This typically includes specific exercises (pelvic floor, core, stretching), manual therapy techniques, education on body mechanics and lifestyle modifications, and strategies for symptom management.
- Education and Home Exercise Programme: A significant component involves education about your condition and self-management strategies. You will be taught specific exercises to perform at home and receive guidance on proper technique, frequency, and progression to ensure continued progress between sessions. Questions are encouraged throughout the process.
Benefits of Postpartum Pelvic Floor Physical Therapy

Postpartum pelvic floor physical therapy offers benefits like improved function, reduced discomfort, and enhanced quality of life, while also providing self-care knowledge and tools.
- Improved Bladder and Bowel Control: Targeted exercises strengthen and coordinate the pelvic floor muscles, significantly reducing or eliminating stress urinary incontinence (leakage with cough/sneeze/exercise), urge incontinence (sudden urge), and faecal incontinence. This improves confidence and reduces reliance on pads.
- Reduction in Pelvic Pain: Physical therapy addresses various sources of postpartum pain, including perineal scar pain, pain with intercourse (dyspareunia), pelvic girdle pain, and low back pain, through manual therapy, exercise, and pain management education, restoring comfort during daily activities.
- Enhanced Core Strength and Stability: Rehabilitating the deep core muscles, including addressing diastasis recti, improves trunk stability, reduces back pain, enhances posture, and provides better support for internal organs and the spine during lifting and movement required for infant care.
- Management and Prevention of Pelvic Organ Prolapse: Strengthening the pelvic floor provides better support for pelvic organs (bladder, uterus, rectum), which can help manage existing mild to moderate prolapse symptoms (feelings of heaviness or bulging) and potentially reduce the risk of future progression.
- Improved Sexual Function: By addressing pelvic floor muscle tension, scar tissue restrictions, and pain, physical therapy can help restore comfortable and pleasurable sexual activity, addressing common postpartum concerns like dyspareunia and altered sensation.
- Safer Return to Exercise and Activity: Therapists provide guidance on modifying activities and gradually progressing exercise intensity, ensuring the body is ready for increased demands. This lowers the risk of injury or worsening of symptoms like incontinence or prolapse upon returning to fitness routines.
- Increased Body Awareness and Empowerment: Physical therapy sessions provide valuable education about pelvic anatomy and function. Learning how to correctly activate and relax pelvic floor and core muscles empowers individuals with tools for long-term self-management and body awareness, promoting confidence in their physical capabilities.
When to Seek Postpartum Pelvic Floor Physical Therapy
Assessment around 6-8 weeks postpartum is beneficial, but seeking help is always possible. Pelvic floor physical therapist evaluations can address specific concerns and optimize recovery.
- Urinary or Faecal Incontinence: Experiencing any involuntary leakage of urine or stool, whether it occurs with coughing, sneezing, laughing, exercise, or associated with a strong urge, warrants an assessment. This is common but not considered normal function long-term.
- Pelvic Pain: Persistent pain in the pelvic region, including perineal pain (especially if related to tearing or episiotomy scars), pain during or after intercourse, tailbone pain (coccydynia), pubic symphysis pain, or deep pelvic ache, should be evaluated.
- Symptoms of Pelvic Organ Prolapse: Feelings of heaviness, pressure, or bulging in the vagina, or the sensation that something is falling out, are potential indicators of prolapse and benefit from a physical therapy assessment for management strategies.
- Persistent Low Back, Hip, or Pelvic Girdle Pain: If pain in these areas persists beyond the initial weeks postpartum and interferes with daily activities or infant care, physical therapy can help identify and address underlying musculoskeletal contributions, such as core weakness or joint dysfunction.
- Concerns about Diastasis Recti or Core Weakness: If you notice a visible gap or doming along the midline of your abdomen, feel significant core weakness, or struggle with functional tasks due to poor core stability, a therapist can assess DRA and guide appropriate rehabilitation.
Postpartum recovery is crucial, and pelvic health physical therapy is a valuable tool for rehabilitating the pelvic floor and core musculature. This therapy addresses common issues like incontinence, pain, diastasis recti, and pelvic organ prolapse. It offers evidence-based strategies, personalized exercise programs, and manual techniques to facilitate optimal healing, restore function, and improve quality of life. Prioritizing pelvic health through physical therapy enhances comfort and confidence in the postpartum journey.
For individuals in Ontario seeking assessment and treatment for postpartum pelvic health concerns, PARC Ontario offers services across multiple locations. Addressing symptoms early can contribute significantly to long-term well-being. You can reach us for inquiries or appointments at the following numbers based on location: (416) 445-2075 or (416) 430-0314 [Scarborough], (905) 897-2092 [Mississauga], (905) 686-9081 [Ajax], (905) 430-2112 [Whitby], and (905) 579-9938 [Oshawa].