Urinary Incontinence: Physical Therapy Solutions and Tips for Women
Urinary incontinence (UI) involves the involuntary leakage of urine. It is a common health concern affecting a significant number of women globally and within Canada. The Canadian Continence Foundation notes that millions of Canadians experience some form of incontinence, with women being disproportionately affected, particularly as they age or after childbirth. This condition can substantially influence a woman’s emotional well-being, social interactions, and physical activities, often leading to reduced confidence and avoidance of certain situations.
This article outlines physical therapy approaches and practical strategies for managing UI in women. Understanding the condition and available treatments is crucial for regaining control. Urinary incontinence is often highly manageable, and effective help is accessible. Seeking appropriate care can lead to significant improvements in symptoms and overall quality of life, empowering women to live more freely and confidently.
Different Types of Urinary Incontinence
Urinary incontinence presents in several distinct forms, each with characteristic symptoms and underlying mechanisms. Identifying the specific type of UI is fundamental for determining the most appropriate management strategy. Physical therapists conduct thorough assessments to differentiate between these types and tailor treatment plans accordingly. Understanding these variations helps women recognize their symptoms and communicate effectively with healthcare providers.
- Stress Urinary Incontinence (SUI)
This type involves urine leakage during activities that increase abdominal pressure, such as coughing, sneezing, laughing, lifting, or exercising. It often results from weakened pelvic floor muscles or urethral sphincter insufficiency, failing to provide adequate support to prevent urine loss during these physical exertions.
- Urge Urinary Incontinence (UUI)
Also known as overactive bladder (OAB) with incontinence, UUI is characterized by a sudden, intense urge to urinate, immediately followed by involuntary urine loss. The bladder muscle contracts involuntarily, often before an individual can reach a washroom. Triggers can include the sound of running water or arriving home.
- Mixed Urinary Incontinence
Many women experience symptoms of both stress and urge incontinence simultaneously. This combination, termed mixed urinary incontinence, involves leakage associated with both physical exertion or pressure and sudden, strong urges to urinate. Management typically requires addressing both components of the condition.
- Overflow Incontinence
This form occurs when the bladder does not empty completely, leading to frequent or constant dribbling of urine. It results from an underactive bladder muscle or a blockage preventing normal urine flow. Individuals may feel like their bladder is never fully empty after urinating.
- Functional Incontinence
Functional incontinence arises when physical or cognitive impairments prevent an individual from reaching the toilet in time, despite normal bladder function. Conditions like severe arthritis, mobility issues, or neurological disorders such as dementia can contribute to this type of incontinence by hindering timely access to facilities.
Common Causes and Risk Factors for UI in Women

A variety of factors can contribute to the development or worsening of urinary incontinence in women. These involve physiological changes, lifestyle elements, and underlying medical conditions that affect the structures supporting bladder control, namely the pelvic floor muscles, nerves, and connective tissues. Recognizing these potential contributors is important for prevention and effective management.
- Pregnancy and Childbirth
- The physical stresses of pregnancy and vaginal delivery can significantly impact pelvic floor muscles and nerves. Hormonal changes during pregnancy, the weight of the growing uterus, and the strain of labour can weaken supportive structures, increasing the likelihood of developing stress incontinence postpartum or later in life.
- Menopause and Ageing
Declining oestrogen levels during menopause can lead to thinning and reduced elasticity of tissues in the urethra and bladder lining, potentially weakening urinary control mechanisms. Natural ageing processes also contribute, as pelvic floor muscles may gradually lose strength and tone over time, increasing susceptibility to UI.
- Pelvic Organ Prolapse (POP)
This medical condition develops when the rectum, uterus, or bladder drop out of their natural places, possibly putting pressure on the urethra or bladder. POP often results from weakened pelvic floor support structures and can directly contribute to both stress and urge incontinence symptoms.
- Obesity
Excess body weight increases pressure on the bladder and surrounding pelvic floor muscles. This chronic strain can weaken these structures over time, contributing significantly to the development or exacerbation of stress urinary incontinence. Weight management is often a component of UI treatment plans.
- Hysterectomy and Pelvic Surgery
Surgical procedures involving the pelvic region, such as hysterectomy (removal of the uterus), can sometimes damage nerves or alter the anatomical support structures related to bladder control. This potential disruption can lead to the onset or worsening of urinary incontinence post-surgery.
- Chronic Conditions
Certain medical conditions elevate the risk of UI. Chronic constipation leads to straining, which stresses the pelvic floor. Chronic coughing (due to smoking or respiratory disease) exerts repeated pressure. Neurological disorders like multiple sclerosis or Parkinson’s disease can impair nerve signals controlling the bladder. Diabetes can cause nerve damage affecting bladder function.
- Lifestyle Factors
Certain lifestyle choices can influence bladder health. Consuming bladder irritants like caffeine, alcohol, or acidic foods may worsen urge incontinence symptoms. Smoking contributes to chronic coughing, increasing stress incontinence risk. Inadequate fluid intake can concentrate urine, irritating the bladder, while excessive fluid intake increases urine volume.
How Physical Therapy Can Help Manage Urinary Incontinence
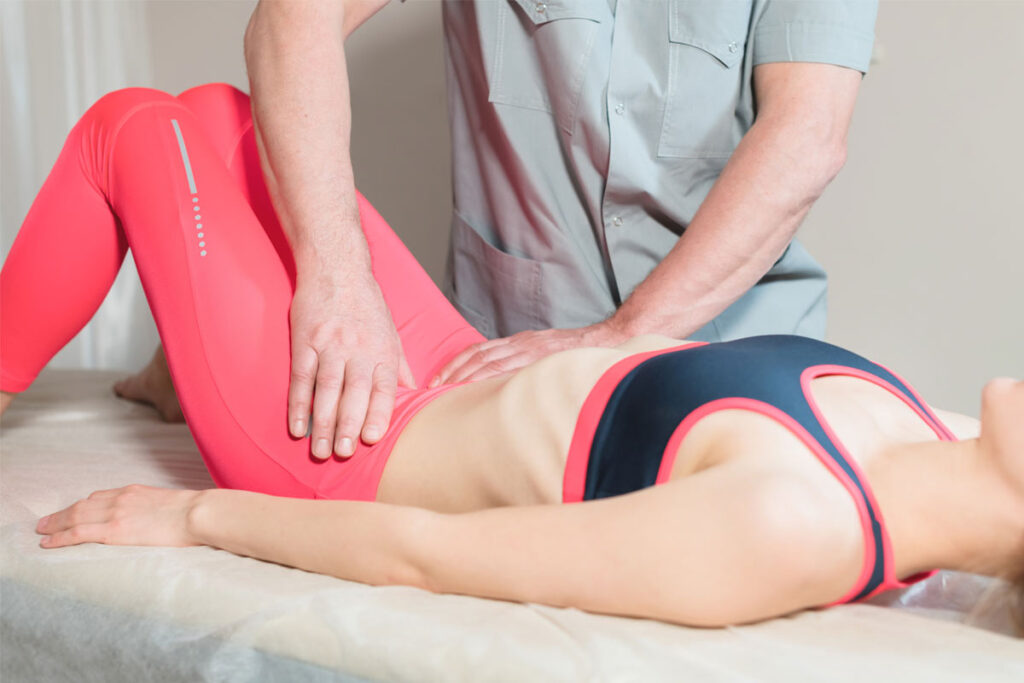
Physical therapy, often termed pelvic health physiotherapy in this context, plays a central role in the conservative management of urinary incontinence for many women. It offers non-surgical, evidence-based strategies focused on restoring function to the pelvic floor muscles and improving bladder control habits.
- Detailed Assessment
Physiotherapists conduct thorough evaluations, including pelvic floor muscle checks, to understand the specific type and cause of incontinence. This assessment identifies muscle strength, coordination deficits, or tension patterns, guiding a personalized treatment plan for effective management and symptom relief tailored to individual needs.
- Pelvic Floor Muscle Training (PFMT)
Therapy focuses on teaching correct identification and execution of pelvic floor exercises (Kegels). Strengthening these muscles provides better support for the bladder and urethra, improving closure mechanisms during activities that increase abdominal pressure, thereby reducing stress incontinence leakage effectively.
- Biofeedback Utilization
Biofeedback employs sensors providing real-time information on pelvic floor muscle activity. This visual or auditory feedback enhances body awareness, helping patients learn to properly contract and relax these muscles, improving control and coordination essential for managing both stress and urge incontinence symptoms.
- Electrical Stimulation Application
For individuals with very weak muscles or difficulty initiating contractions, gentle electrical stimulation can be used via a probe. This passively activates pelvic floor muscles, helping to re-educate the neuromuscular pathways, build strength, and improve muscle responsiveness necessary for bladder control support.
- Bladder Retraining Strategies
Physiotherapists implement structured bladder retraining programmes, particularly for urge incontinence. This involves scheduled voiding, gradually increasing intervals between urination, and teaching urge suppression techniques. The goal is to restore normal bladder capacity and reduce urinary frequency and urgency over time.
- Core Stability Enhancement
Treatment often includes exercises targeting deep abdominal, back, and diaphragm muscles. Strengthening the entire core musculature improves overall pelvic stability and support, complementing pelvic floor function and contributing significantly to better bladder control and reduced incontinence episodes during movement or exertion.
- Lifestyle Adjustments Guidance
Therapists provide advice on modifying lifestyle factors contributing to UI. This includes optimizing fluid intake, identifying and managing dietary bladder irritants (like caffeine), ensuring regular bowel movements to prevent straining, and teaching techniques for safe lifting and daily activities management.
- Patient Education Empowerment
Education is key. Physiotherapists explain pelvic anatomy, bladder function, and the specific reasons behind an individual’s incontinence. Understanding the condition and learning self-management techniques empowers patients to actively participate in their recovery and maintain long-term improvements in bladder control.
Practical Tips and Lifestyle Modifications for Women with UI
Incorporating specific lifestyle adjustments and practical tips into daily routines can significantly help manage urinary incontinence symptoms alongside formal treatments like physiotherapy.
- Manage Fluid Intake Wisely
Stay hydrated but avoid drinking large amounts at once. Sip fluids throughout the day. Limit drinks before bedtime or activities where washrooms are inaccessible. Reduce intake of caffeine and alcohol, as these can irritate the bladder and increase urgency.
- Identify Dietary Triggers
Note foods that may worsen symptoms. Common irritants include caffeine, alcohol, spicy foods, acidic fruits/juices, and artificial sweeteners. Try eliminating potential triggers one by one to see if symptoms improve, then adjust your diet accordingly for better bladder comfort.
- Practise Timed Voiding
Schedule regular trips to the washroom, perhaps every 2-4 hours, even if you don’t feel a strong urge. This helps prevent the bladder from becoming overly full, reducing the risk of urgency-related leaks and helping to retrain bladder habits.
- Maintain a Healthy Weight
Excess body weight increases pressure on the bladder and pelvic floor muscles, potentially worsening stress incontinence. Achieving and maintaining a healthy weight through balanced nutrition and regular, appropriate exercise can significantly reduce this pressure and improve symptoms.
- Prevent Constipation
Straining during bowel movements puts stress on the pelvic floor. Ensure adequate fibre intake from fruits, vegetables, and whole grains, drink sufficient water, and stay active to promote regular, easy bowel movements and reduce pelvic floor strain.
- Use Proper Lifting Techniques
When lifting heavy objects, engage your core and pelvic floor muscles beforehand. Bend at the knees, not the waist, keeping the object close to your body. Exhale during the exertion phase to minimize downward pressure on the pelvic organs.
- Choose Appropriate Clothing and Products
Wear clothing that is easy to remove quickly if urgency is an issue. Use absorbent incontinence pads or protective underwear designed for urine leakage. These products offer discretion and security, helping you maintain confidence during daily activities.
Urinary incontinence is a prevalent condition that can significantly affect women’s lives, but it is not an inevitable consequence of ageing or childbirth. Effective management strategies are available, with pelvic health physiotherapy offering a robust, non-invasive approach. Through targeted exercises, behavioural modifications, and education, physical therapy addresses the underlying muscular and functional factors contributing to UI, helping women regain confidence and control over their bladder function.
Seeking professional guidance is a positive step towards managing symptoms and improving quality of life. If you are experiencing urinary incontinence, consider consulting with healthcare providers experienced in pelvic health. For residents in specific Ontario regions seeking physiotherapy and related rehabilitation services, contact PARC Ontario. We have various locations and can be reached at the following numbers: (416) 445-2075 or (416) 430-0314 [Scarborough], (905) 897-2092 [Mississauga], (905) 686-9081 [Ajax], (905) 430-2112 [Whitby], and (905) 579-9938 [Oshawa]. Taking action can lead to significant improvements in managing urinary incontinence.